Marker Name: BUN
REFERENCE RANGES FOR BUN:
Laboratory reference range: 6–24 mg/dL
Functional reference range: 13–18 mg/dL
DESCRIPTION:
Urea is a water-soluble end product of protein metabolism suitable for excretion in the urine.1 BUN, or blood urea nitrogen, is the quantity of urea nitrogen in the blood. Urea provides no known physiologic benefit in humans other than as a waste product. Nevertheless, BUN is a clinically useful laboratory test that is measured in essentially every person who receives an order for routine blood work.2,3
Urea is created by the urea cycle, also known as the ornithine cycle.4 The liver is the primary source of urea production, but some urea production also takes place in the kidneys and intestines. Nitrogen found in urea may derive from ingested proteins or muscle catabolism.1 Each molecule of urea contains two nitrogen atoms, one from ammonia and one from aspartate, combined by the enzyme arginase.5 Urea cycle function is dependent on activation of carbamoyl phosphate synthase by N-acetylglutamate.6 After it is synthesized, urea passively diffuses across cell membranes and is found in the bloodstream.7 Urea is excreted by the kidney or, to a smaller degree, in sweat. BUN levels increase approximately 50 percent from infancy to adulthood, and BUN levels tend to be slightly higher in men than in women.8,9
BUN varies inversely with glomerular filtration rate. That is, increases in BUN correlate with decreases in kidney function.10 However, BUN is not a precise measure of glomerular filtration rate for two reasons.10 First, the rate of urea production is not constant and may increase substantially in patients who consume high-protein diets or in the context of increased tissue catabolism. Conversely, a low-protein diet or liver disease may decrease BUN apart from kidney function. Second, roughly half of filtered urea by the glomerulus is passively absorbed in the proximal tubules. Thus, BUN will vary as sodium and water reabsorption rates change. For these reasons, creatinine levels in blood are a far more accurate measure of glomerular filtration rate and overall kidney function.
As a clinical tool, BUN is most useful when interpreted in the context of blood creatinine levels. Under normal conditions, the ratio of BUN to creatinine is between 10:1 and 20:1. If the BUN-to-creatinine ratio exceeds 20:1, it indicates prerenal injury and, most often, decreased renal perfusion.11,12
BUN is also useful for estimating glomerular filtration rate in advanced kidney failure.13 In advanced kidney disease, creatinine clearance overestimates kidney function while urea clearance underestimates it. Therefore, glomerular filtration rate can be more accurately estimated in advance kidney failure by averaging clearance rates of both molecules.14
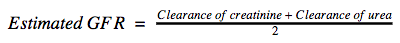
Elevated levels of urea in the blood may be referred to as uremia or azotemia. Uremia generally reflects a more severe clinical state in which various blood electrolytes are abnormal beyond BUN. Uremia is often used interchangeably with end-stage renal disease or advanced kidney failure.15 Azotemia, on the other hand, reflects a broad set of etiologies for mild to moderate BUN elevations. Azotemia is sometimes used interchangeably with the term prerenal disease, or, simply prerenal azotemia.16 The most common causes of elevated BUN include decreased renal perfusion, acute or chronic kidney disease, or medications. In fact, a large number of medications across various drug classes may increase BUN.8,10
An abnormally low BUN in isolation is rarely a cause for concern. While decreased BUN may occur in the context of severe liver disease, this state is usually obvious from other clinical and laboratory evidence. BUN may also be low from excessive hydration (e.g., primary polydipsia, iatrogenic). A low BUN usually reflects a low-protein diet or is a side effect from drugs such as chloramphenicol and streptomycin.
BUN is always measured with creatinine, and these two values are the primary ways to estimate glomerular filtration rate and kidney function.10 BUN is measured as part of the basic metabolic panel or complete metabolic panel. Depending on the clinical situation, BUN may also be measured with blood ammonia levels and urinalysis.
PATHOLOGICAL/CONVENTIONAL RANGE INDICATIONS:
High in:8,17-19
- Hypovolemia/dehydration
- High-protein diet
- Total parenteral nutrition
- Gastrointestinal hemorrhage
- Ketoacidosis
- Kidney diseases
- Glomerulonephritis (acute or chronic)
- Pyelonephritis
- Acute tubular necrosis
- Interstitial nephritis
- End-stage renal disease
- Ureteral obstruction
- Shock
- Congestive heart failure
- Thermal burn injury
- Recent heart attack
- Drugs
- Diuretics (e.g., furosemide, hydrochlorothiazide)
- Antibiotics (e.g., tetracyclines)
- Anti-gout medications (e.g., allopurinol, probenecid)
- Chemotherapeutics (e.g., cisplatin)
Low in:8
- Low-protein diet
- Malnutrition
- Excessive fluid administration
- Polydipsia
- Drugs
- Streptomycin
- Chloramphenicol
FUNCTIONAL RANGE INDICATIONS:
High in:
- Mild dehydration
- Impaired kidney function
- Inadequate sodium intake
- Stress
- Hypochlorhydria
- Urinary tract obstruction
Low in:
- Impaired liver function
- Poor nutrient status/malabsorption
- Celiac disease
- Hypochlorhydria
- Anabolic steroid use
- Impaired kidney function
References:
- http://www.uptodate.com/contents/urea-cycle-disorders-clinical-features-and-diagnosis
- http://www.ncbi.nlm.nih.gov/pmc/articles/PMC1025851/
- http://www.clinchem.org/content/12/3/137.abstract
- http://physrev.physiology.org/physrev/70/3/701.full.pdf
- http://www.uptodate.com/contents/image?imageKey=PEDS%2F60652&topicKey=ALLRG%2F2929&rank=2%7E150&source=see_link&search=BUN
- http://www.ncbi.nlm.nih.gov/pubmed?term=20227314
- http://www.ncbi.nlm.nih.gov/books/NBK21626/
- http://emedicine.medscape.com/article/2073979-overview#a2
- http://www.ncbi.nlm.nih.gov/pubmed?term=16760447
- http://www.uptodate.com/contents/assessment-of-kidney-function
- http://www.ncbi.nlm.nih.gov/pubmed/?term=10779250
- http://ckj.oxfordjournals.org/content/5/2/187.abstract
- http://ndt.oxfordjournals.org/content/20/suppl_9/ix3.short
- http://www.ncbi.nlm.nih.gov/pubmed?term=6071183
- http://www.uptodate.com/contents/overview-of-the-management-of-chronic-kidney-disease-in-adults
- http://www.ncbi.nlm.nih.gov/pubmed/12549657
- https://nlm.nih.gov/medlineplus/ency/article/003474.htm
- http://www.uptodate.com/contents/etiology-and-diagnosis-of-prerenal-disease-and-acute-tubular-necrosis-in-acute-kidney-injury-acute-renal-failure
- http://www.ncbi.nlm.nih.gov/pubmed/16932399