Marker Name: eGFR
REFERENCE RANGES FOR eGFR:
Laboratory reference range: >59 mL/min/1.73
DESCRIPTION:
eGFR stands for estimated glomerular filtration rate. The overall glomerular filtration rate equals the sum of filtration rates from each functioning nephron. The precise measurement of glomerular filtration rate is complex, time-consuming, and impractical to perform in routine clinical practice.1 Moreover, an exact GFR is not needed for most clinical scenarios. Therefore, an approximate glomerular filtration rate is estimated from routine laboratory testing. Levels of creatinine in the blood are the most commonly used method to estimate GFR.1
Almost all endogenous creatinine comes from skeletal muscle and is produced at a constant rate.2 Creatinine is freely filtered by the glomerulus and is not reabsorbed, secreted, or metabolized by the nephron.3 In most circumstances, an increase in serum levels of creatinine reflects a decrease in glomerular filtration rate, and vice versa.4
Since the 1970s, clinicians have estimated GFR from serum creatinine using the Cockcroft-Gault equation.5
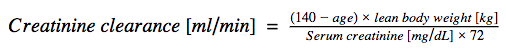
Because women generally have less lean muscle mass than men, the result of the equation is multiplied by 0.85 when estimating GFR in women. While the Cockcroft-Gault equation was the main means of estimating GFR from serum creatinine, authors of the MDRD study published a revised equation that apparently provides a more accurate estimate.6 The mathematics of the MDRD equation are more complex than Cockcroft-Gault, thus it is more convenient to use an online calculator.7 In people with chronic kidney disease, a separate equation, called the CKD- EPI, is more accurate.8
A more precise but still estimated GFR can be determined by using urinary excretion of inulin. Inulin is physiologically inert, freely filtered at the glomerulus, and not secreted, reabsorbed, or metabolized by the kidney.9 As such, it is the ideal molecule for estimating GFR. Unfortunately, inulin is rather expensive and difficult to assay and is rarely used clinically.1 Urine creatinine clearance is often used as a surrogate, since creatinine nearly fulfills the same criteria.10 Urinary creatinine times the total volume of urine produced in 24 hours divided by serum creatinine provides a reasonably accurate estimate of GFR.11
Cystatin C is a low-molecular-weight protein that is filtered by the glomerulus but not reabsorbed. While some researchers and clinicians have tried to find ways to use serum cystatin C as a more accurate means to estimate GFR, attempts have been limited, since cystatin C is partially metabolized in the renal tubules.1
Glomerular filtration rates that exceed normal limits are rarely a clinical problem by themselves. Abnormally high eGFR may represent low muscle mass, since little creatinine is being created by muscle.12 Protein malnutrition and advanced liver disease may lead to lower creatinine levels, and, by extension, elevated eGFR.
Low eGFR occurs in a wide range of clinical conditions. Reduced glomerular filtration rates are usually caused by conditions that directly or indirectly affect the kidney. The main indirect cause of reduced GFR is poor blood flow to the kidney, whether due to hypovolemia, congestive heart failure, or some other cardiovascular condition. Chronic elevations in eGFR usually reflect primary disease of the kidney. In fact, eGFR plays a key role in staging chronic kidney disease.13 The five stages of chronic kidney disease are stratified by progressively increasing ranges of eGFR.
eGFR is now automatically calculated from serum creatinine and presented in the results of each basic metabolic panel or complete metabolic panel.1 There are usually two results listed, one calculated assuming the patient is African-American and the other assuming the patient is not, since race affects the normal range for GFR.
PATHOLOGICAL/CONVENTIONAL RANGE INDICATIONS:
High in:12
- Low muscle mass
- Liver failure
- Protein malnutrition
Low in:14-16
- Hypovolemia/dehydration
- Shock
- Chronic kidney disease
- Glomerular (e.g., Goodpasture syndrome)
- Vascular (e.g., hypertensive nephrosclerosis)
- Tubulointerstitial (e.g., urinary tract infection, renal calculi)
- Cystic (e.g., polycystic kidney disease)
- Diabetic (e.g., diabetic nephropathy)
- Transplant (e.g., rejection, anti-rejection drug toxicity)
- Acute interstitial nephritis
- Acute glomerulonephritis
- Prerenal azotemia
- Acute tubular necrosis
- Metabolic acidosis
- Diabetic ketoacidosis
- Alcoholic ketoacidosis
- Gastrointestinal bleeding
- Sickle cell anemia
- Rhabdomyolysis
- Multiple myeloma
FUNCTIONAL RANGE INDICATIONS:
High in:
- No functional range
Low in:
- No functional range
References:
- http://www.uptodate.com/contents/assessment-of-kidney-function
- http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4460282/
- https://books.google.com/books/about/Renal_Physiology.html?id=1te7M5Cn79EC
- http://www.uptodate.com/contents/reciprocal-serum-creatinine-concentration-and-chronic-kidney-disease
- http://www.ncbi.nlm.nih.gov/pubmed?term=1244564
- http://dx.doi.org/10.7326/0003-4819-145-4-200608150-00004
- http://nephron.org/mdrd_gfr_si
- http://www.niddk.nih.gov/health-information/health-communication-programs/nkdep/lab-evaluation/gfr-calculators/adults-conventional-unit-ckd-epi/Pages/default.aspx
- http://www.ncbi.nlm.nih.gov/pubmed?term=10100067
- http://www.clinchem.org/content/38/10/1933.abstract
- http://dx.doi.org/10.1016/0140-6736(92)92502-7
- http://emedicine.medscape.com/article/2054342-overview#showall
- http://www.uptodate.com/contents/definition-and-staging-of-chronic-kidney-disease-in-adults
- http://www.ncbi.nlm.nih.gov/pubmed/22445471
- http://www.ncbi.nlm.nih.gov/pubmed/16825087
- http://www.ncbi.nlm.nih.gov/pubmed/11904577