Marker Name: Hematocrit
REFERENCE RANGES FOR HEMATOCRIT:
Laboratory reference range:
Male and Female: 37.5–51%
Functional reference ranges:
Male: 40–48%
Female: 37–44%
DESCRIPTION:
Hematocrit (Hct) is the percentage of red blood cells, by volume, in the blood. Thus, hematocrit provides information about the relative amount of red blood cells per unit of blood volume. The main function of a red blood cell (erythrocyte) is to deliver oxygen to tissues throughout the body. Its unique torus shape is ideal for gas diffusion, and it is flexible enough to pass through small capillaries in peripheral tissues.1 Red blood cells are also important for the removal of carbon dioxide from the tissues and can help buffer the pH of the blood.
Erythropoiesis, or the production of new red blood cells, takes place in the bone marrow.2 Red blood cells are only one possible cell type that may be formed from pluripotent stem cells; the stem cells also give rise to all of the white blood cells and platelets. Erythropoiesis requires the coordination of numerous cytokines and hormones. Perhaps the most important hormone for red cell production is erythropoietin, which is produced in the kidney.3 Immature red blood cells called reticulocytes move from the bone marrow into the vasculature, where they take about one week to mature into fully functional erythrocytes.2 A mature red blood cell circulates in the blood stream for approximately 120 days, after which it is removed from the bloodstream by macrophages.4,5
Modern instruments calculate hematocrit (Hct) by directly counting the number of red blood cells in a sample and multiplying it by the mean corpuscular volume (MCV) using the following equation:
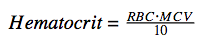
A high hematocrit is called erythrocytosis or polycythemia. A high hematocrit may be due to an increased number of red blood cells (true erythrocytosis) or a normal number of red blood cells in blood with an elevated mean corpuscular volume.6 Since hematocrit is the volume of packed red blood cells per unit of blood volume, it may be elevated when there are too many red blood cells or too little plasma. An elevated hematocrit caused by too many red blood cells may be congenital polycythemia, primary polycythemia (also known as polycythemia vera), secondary polycythemia, or idiopathic erythrocytosis. Causes of secondary polycythemia range from simple hypoxia to certain forms of cancer, such as leukemia. Less commonly, elevated hematocrit may be caused by an abnormally low plasma volume. This condition most commonly occurs in people who smoke.
A low hematocrit is synonymous with anemia. A low hematocrit may occur through one of four ways: blood loss, decreased red blood cell production, increased red blood cell destruction, or an increase in plasma volume. Some people may have a chronically low hematocrit from birth, as is the case in glucose-6 phosphate dehydrogenase deficiency. Blood loss may be rapid, such as after severe trauma with hemorrhage, or it may be slow, such as chronic gastrointestinal bleeding. Various forms of cancer are the most common cause of decreased red blood cell production. Red blood cells may be destroyed by parasites (as seen in malaria) or as a consequence of genetic disease (e.g., sickle cell anemia).
Hematocrit is measured as a part of a complete blood count (CBC), which includes hemoglobin, hematocrit, a red blood cell (RBC) count, mean corpuscular volume (MCV), mean corpuscular hemoglobin (MCH), mean corpuscular hemoglobin concentration (MCHC), and red cell distribution width (RDW).7 The complete blood count may also include a reticulocyte count. It is often measured with related iron markers, including TIBC, UIBC, iron saturation, serum iron, and ferritin.
PATHOLOGICAL/CONVENTIONAL RANGE INDICATIONS:
High in:8-14
- Dehydration
- Decreased plasma volume in relation to red blood cells (hemoconcentration)
- Smoker’s polycythemia
- Gaisbock’s disease (stress erythrocytosis)
- Polycythemia vera (primary polycythemia)
- Idiopathic erythrocytosis
- Secondary polycythemia
- Hypoxia
- Obstructive sleep apnea
- Pulmonary fibrosis
- Chronic obstructive pulmonary disease (COPD)
- Erythropoietin-secreting tumor (e.g., hepatocellular carcinoma, renal cell carcinoma, hemangioblastoma, pheochromocytoma, uterine myomata)
- Congenital polycythemia
- Treatment with erythropoietin
Low in:7,15,16
- First and second trimesters of normal pregnancy
- Nutrient imbalance
- Iron deficiency
- Folate deficiency
- Vitamin B12 deficiency
- Vitamin B6 deficiency
- Copper deficiency
- Heavy menstrual periods
- Serial phlebotomy
- Excessive fluid intake (polydipsia)
- Excessive fluid administration (iatrogenic; dilution anemia)
- Chronic inflammation (e.g., chronic infection, malignancy, rheumatologic disorders, inflammatory bowel disease, chronic immune activation)
- Sideroblastic anemia
- Hemorrhage
- Internal
- External
- Red blood cell destruction
- Sickle cell anemia
- Thalassemia
- Autoimmune hemolytic anemia
- Evans syndrome
- Malaria
- Bartonella
- Leptospirosis
- Bone marrow suppression
- Primary bone marrow failure
- Certain cancers
- Leukemia
- Gastric adenocarcinoma
- Adenocarcinoma of the cecum
- Certain genetic conditions
- Glucose-6 phosphate dehydrogenase deficiency
- Drugs
- Cephalosporins
- Chemotherapeutic agents
FUNCTIONAL RANGE INDICATIONS:
High in:
- Dehydration
- Erythrocytosis
- Polycythemia
Low in:
- Functional anemia
References:
- http://www.physics.uoguelph.ca/~dutcher/download/handbook%20of%20biological%20physics/1.pdf
- http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3684002/
- http://www.ncbi.nlm.nih.gov/pubmed/?term=12524467%5Buid%5D
- http://www.ncbi.nlm.nih.gov/pubmed/?term=16193055
- http://www.ncbi.nlm.nih.gov/pubmed/?term=10571815%5Buid%5D
- http://www.uptodate.com/contents/automated-hematology-instrumentation
- http://www.uptodate.com/contents/approach-to-the-adult-patient-with-anemia
- http://www.ncbi.nlm.nih.gov/pubmed/?term=23457296
- http://www.uptodate.com/contents/diagnostic-approach-to-the-patient-with-polycythemia
- http://www.ncbi.nlm.nih.gov/pubmed/?term=9358074
- http://www.ncbi.nlm.nih.gov/pubmed/?term=5545457%5Buid%5D
- http://www.ncbi.nlm.nih.gov/pubmed/?term=7567437
- http://www.ncbi.nlm.nih.gov/pubmed/?term=9292543%5Buid%5D
- http://www.ncbi.nlm.nih.gov/pubmed/?term=618465
- https://www.nlm.nih.gov/medlineplus/ency/article/000578.htm
- http://www.ncbi.nlm.nih.gov/pubmed/?term=15987327