Marker Name: Free T4
REFERENCE RANGES FOR FREE T4 (THYROXINE):
Laboratory reference range: 0.82–1.77 ng/dL
Functional reference range: 1.0–1.5 ng/dL
DESCRIPTION:
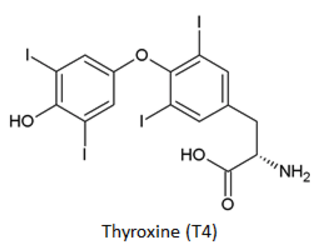
Free T4 is the portion of the total thyroid hormone T4 (thyroxine) pool that is not bound to serum proteins. T4 is the molecular precursor of T3 (triiodothyronine), which is an order of magnitude more potent than T4 at thyroid hormone-responsive receptors.1 The thyroid gland is the only source of T4 synthesis in the body.2 The terms T4 and T3 indicate four and three iodine atoms bound to the core thyroid hormone molecule, respectively.

A substantial amount of T4 is stored within the thyroid gland. Within this gland, most T4 is bound to the protein thyroglobulin within thyroid follicles.2 Thyroid-stimulating hormone stimulates the thyroid gland to hydrolyze thyroglobulin and release free T4, along with other actions that promote thyroid hormone synthesis and secretion.3
Secreted free T4 quickly binds to serum proteins; greater than 99 percent of circulating T4 is bound to a serum protein.4 Approximately 75 percent of T4 in the bloodstream is bound to thyroxine-binding globulin (TBG), 12 percent is bound to albumin, 10 percent is bound to transthyretin, and 3 percent is bound to lipoproteins.2,4 The remaining 0.02 percent of unbound T4, or free T4, is the biologically active portion of serum T4.2
Four different tests are available to estimate free T4. Two of them are routinely used by clinical laboratories, and none of them actually measures free T4 in the serum.5 The first free T4 estimate in common use is the “Free T4 index.” The Free T4 index estimates free T4 from total T4 and the thyroid hormone binding index, which is measured by determining T3 resin uptake. “Direct” free T4 assays estimate free T4 using various methodologies, none of which is a direct measurement.6 The only true direct measurement of free T4 is by equilibrium dialysis, which is only available in reference laboratories and is not routinely used in clinical laboratories because of its cost.5 The major drawback of each of the four laboratory clinical assays is that if the patient has a serum-binding protein abnormality, results are significantly inaccurate.5
Since free T4 is often estimated rather than directly measured, there is a risk that abnormalities in total T4 may be due to abnormalities in TBG levels, rather than true hyperthyroidism or hypothyroidism. When total T4 levels are abnormal, a normal free T4 value suggests an abnormality in TBG levels.5,7 True hyper- or hypothyroidism will be accompanied by elevated or reduced levels of free T4, respectively. In some cases, T4 levels may be abnormally high in the absence of TSH abnormalities or overt signs of hyperthyroidism (e.g., euthyroid hyperthyroxinemia).8 Decreased free T4 levels in the serum usually indicate hypothyroidism or chronic or subacute thyroiditis.
Free T4 may be measured with serum TSH to determine the degree of hypothyroidism or hyperthyroidism.5 Combining the measurement of serum TSH and serum free T4 increases the sensitivity and specificity of thyroid function testing.9 Free T4 may also be measured with total T3, free T3, or reverse T3 in certain circumstances. Patients with suspected autoimmune thyroiditis may be tested for the presence of antibodies against thyroid peroxidase (TPO), thyroglobulin (Tg), and the TSH receptor, along with serum free T4 levels.5
PATHOLOGICAL/CONVENTIONAL RANGE INDICATIONS:
High in:5,10-12
- Pregnancy
- Hyperthyroidism
- Euthyroid hyperthyroxinemia
- TSH-mediated hyperthyroidism
- Acute thyroiditis
- Familial dysalbuminemic hyperthyroxinemia
- Drugs that increase TBG (e.g., estrogens, tamoxifen, opioids)
- Drugs that decrease T4 conversion to T3 (e.g., amiodarone)
Low in:5,10,13
- Hypothyroidism
- Chronic thyroiditis
- Subacute thyroiditis
- Nephrosis
- Congenital thyroid agenesis, dysgenesis, or defects in hormone synthesis
- Synthetic triiodothyronine treatment
- Drugs that decrease TBG (e.g., anabolic steroids, glucocorticoids)
- Drugs that increase T4 clearance (e.g., phenytoin, carbamazepine, phenobarbital)
- Drugs that inhibit T4 synthesis/release (e.g., thionamides, lithium, perchlorate)
FUNCTIONAL RANGE INDICATIONS:
High in:
- Hyperthyroidism
- Facetious hyperthyroidism
Low in:
- Hypothyroidism
- T3 replacement therapy
References:
- http://www.ncbi.nlm.nih.gov/books/NBK285568/
- http://www.uptodate.com/contents/thyroid-hormone-synthesis-and-physiology
- http://www.ncbi.nlm.nih.gov/pubmed?term=1425489
- http://www.ncbi.nlm.nih.gov/pubmed?term=2108013
- http://www.uptodate.com/contents/laboratory-assessment-of-thyroid-function
- http://www.ncbi.nlm.nih.gov/pubmed?term=1582025
- http://www.ncbi.nlm.nih.gov/pubmed/12625976
- http://emedicine.medscape.com/article/118562-overview
- http://dx.doi.org/10.1001/jama.1990.03440110095035
- http://www.mayomedicallaboratories.com/test-catalog/Clinical+and+Interpretive/8724
- http://dx.doi.org/10.1016/j.amjmed.2004.11.028
- http://www.uptodate.com/contents/overview-of-thyroid-disease-in-pregnancy
- http://www.uptodate.com/contents/disorders-that-cause-hyperthyroidism